Think about what happens to you physically when you feel down or sad. You probably experience a loss of energy. Maybe you are exhausted. Possibly you have a headache. Now, what happens when you feel stressed? Your heart races, you might be sweating, or you may be experiencing nausea.
These are just some of the immediate physical responses to your emotions at a stressful, upsetting or unhappy moment that pass once the moment is over. When someone is struggling with a mental health issue like anxiety or depression, these physical responses may be frequent or continuous. Over time, they can result in significant, far-reaching effects on an individual’s physical health.
Moreover, research has found a correlation between mental health and life expectancy. According to an article published by Bradley University, depression, for example, has been linked to a 50 percent increase in a person’s risk of dying from cancer and a 67 percent increase from heart disease. Researchers believe that in part this is due to issues of access to quality health care for people with a mental illness and that people with a mental illness may be less likely to seek out medical care. But they also believe that mental illnesses cause significant wear and tear on the body.
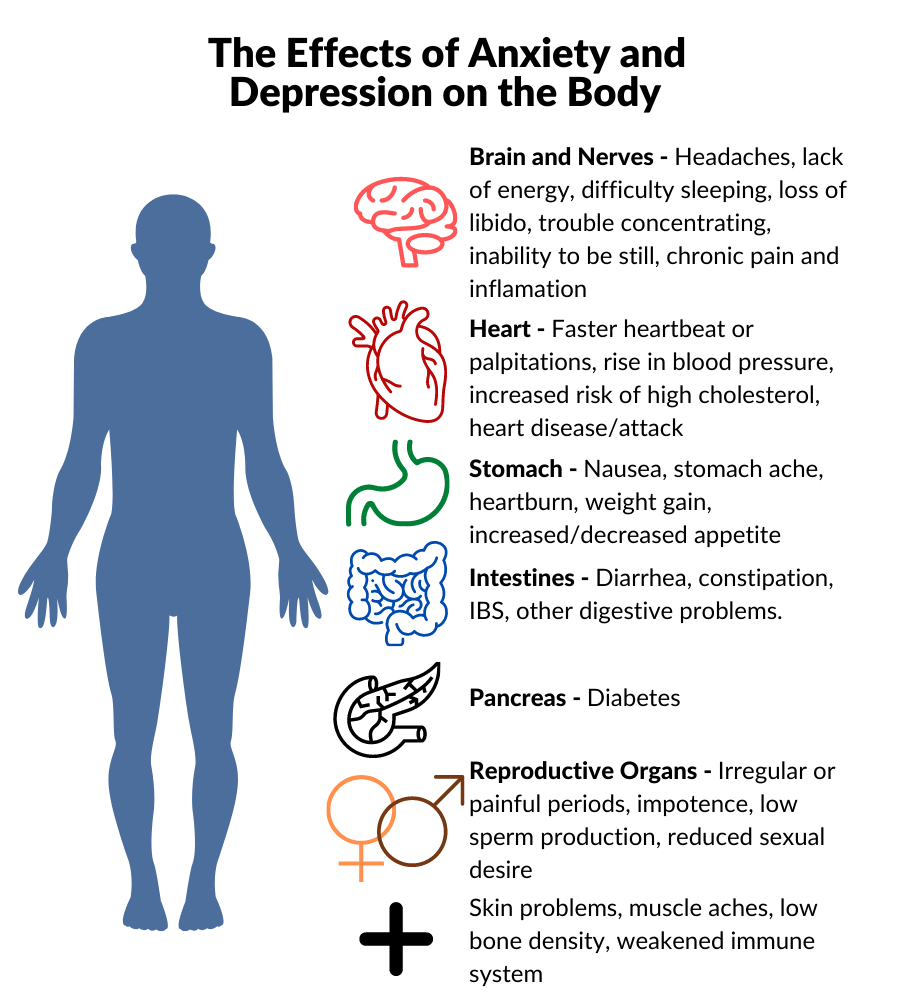
Chronic Stress and the Body
One of the most widely studied mind-body connections is what happens to the body when we experience stress, or the stress response. For someone who is struggling with anxiety or Post Traumatic Stress Disorder and even depression, the stress response is chronically triggered and key biological systems become altered and dysregulated.
There are three interrelated components of the human stress response: catecholamines, HPA axis, and immune system response.
- Catecholamines – These include epinephrine, norepinephrine, and dopamine, which are released by the sympathetic nervous system in response to threat.
- The hypothalamic–pituitary–adrenal (HPA) axis – This system responds with a cascade of stress biochemicals. The hypothalamus releases corticotropin-releasing hormone (CRH), which triggers the pituitary to release adrenocorticotropic hormone (ACTH), finally causing the adrenal glands to activate the flow of cortisol, raising the blood glucose level to respond to threat.
- The immune system –Elevated levels of stress hormones depress immune function. Under normal conditions, the immune system releases proinflammatory cytokines, which increase inflammation to help the body heal wounds and fight infection. Severe and chronic stress causes inflammation levels to be abnormally high, resulting in vulnerability to physical problems and disease.
According to the American Psychological Association, this can cause a long-term drain on all systems of the body. Health issues linked to acute, ongoing stress include chronic pain, respiratory issues such as rapid breathing and asthma, hypertension and heart disease, chronic fatigue and metabolic disorders as well as gastrointestinal issues such as irritable bowel syndrome and ulcers. Heart attacks, strokes, cancer and other serious medical events also are often associated with chronic stress responses.
The good news is, we know that through counseling, therapeutic interventions, self-care and stress-reducing strategies, we can effectively improve the physical health and wellbeing of people with mental health challenges. Some basic beneficial strategies that I work on with my clients include:
- Supporting their communication and relationship skills so they can maintain social and support networks that are so important to their wellbeing.
- Encouraging them to develop healthy routines for exercise, meditation and spending time outside in nature.
- Stressing the importance of getting enough sleep.
These strategies, and others, are key to helping people cope with their feelings and emotions, while at the same time improving their overall physical wellbeing.

